On paper, the United States has everything it needs to end its HIV epidemic. There are powerful medications that can reduce transmission risk to nearly zero, and a once-daily pill called PrEP (Pre-Exposure Prophylaxis) that protects people at risk of contracting the virus. And yet, according to reporting from Vox, the epidemic continues - not because the science failed us, but because the system did.
A preventable gap
Take Brenton Williams, whose story illustrates the frustrating reality for many Americans. His fiancée is HIV positive, making him an ideal candidate for PrEP - exactly the kind of person the medication was designed to protect. But even with health insurance, accessing PrEP wasn't as simple as just asking. Williams described wanting "an extra layer" of protection, a completely reasonable request that shouldn't require navigating bureaucratic hurdles to fulfill.

His experience is far from unique. Despite PrEP being one of the most significant HIV prevention breakthroughs in decades, access remains deeply uneven across the country. Cost, insurance coverage, stigma, and a shortage of informed healthcare providers all create barriers that turn a straightforward medical solution into an obstacle course.
The gap between what's possible and what's real
This is the frustrating heart of the issue. We're not waiting for a medical breakthrough here - the tools already exist. PrEP, when taken consistently, is over 99% effective at preventing HIV from sexual transmission. Combined with other advancements like Undetectable = Untransmittable (U=U), which means people living with HIV who maintain an undetectable viral load cannot transmit the virus to partners, ending the epidemic is theoretically within reach.
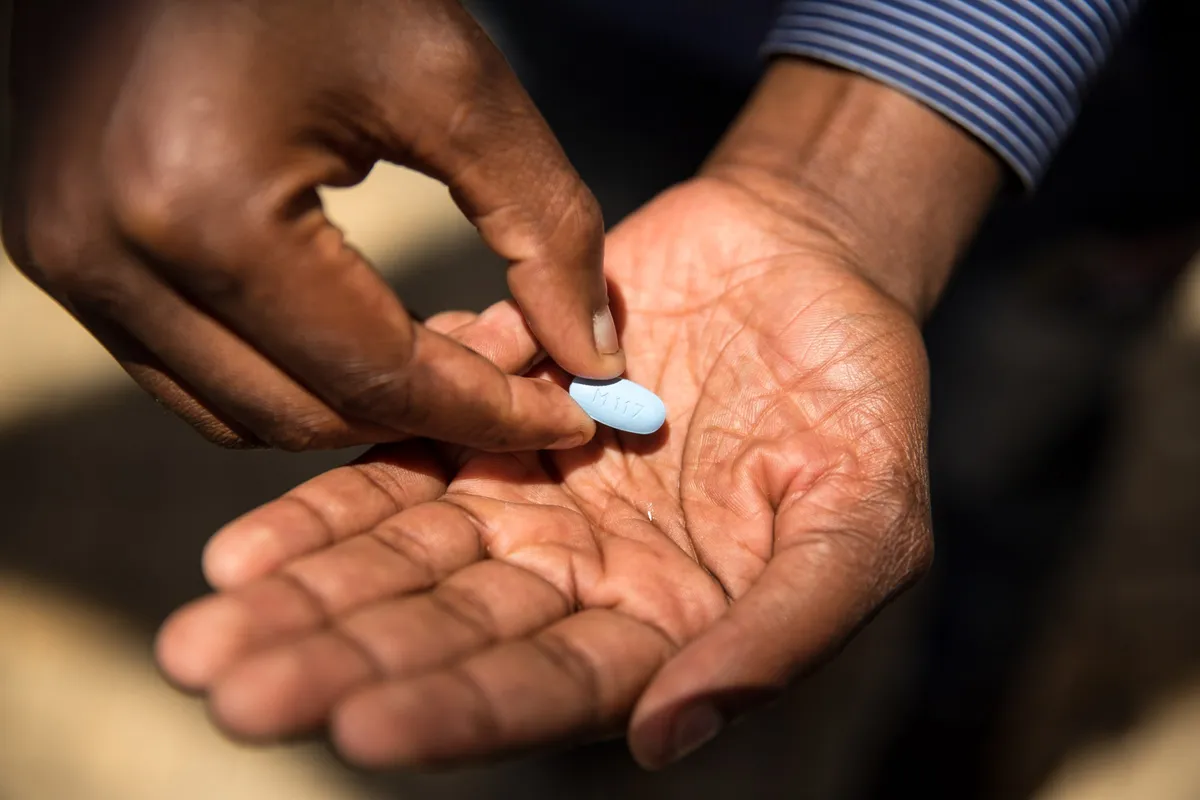
But theory and reality are two different countries. Communities that are disproportionately affected by HIV - including Black and Latino Americans and people in the South - often have the least access to PrEP and HIV care. The medication is there. The awareness frequently isn't. And the healthcare infrastructure to bridge that gap remains inconsistent at best.
Why this matters right now
This isn't just a public health statistic - it's a story about who gets to benefit from medical progress and who gets left behind. When a medication exists that could dramatically reduce new infections and millions of eligible people still can't access it, that's worth paying attention to.

Closing the HIV prevention gap doesn't require a new drug or a new discovery. It requires making the tools we already have genuinely available to the people who need them. That means better insurance coverage, reduced stigma in clinical settings, and more providers educated on prescribing PrEP to at-risk patients.
The science is ready. The question, as Vox's reporting makes clear, is whether the system will catch up.





